
Smart Health: Making Sense of Monkeypox
Questions and answers from an expert about the country’s latest epidemic.
 Last month, monkeypox was declared a public health emergency by the White House. With over 16,000 cases detected in the US—primarily among gay and bisexual men—it is natural for members of the LGBTQ community to feel anxiety and concern.
Last month, monkeypox was declared a public health emergency by the White House. With over 16,000 cases detected in the US—primarily among gay and bisexual men—it is natural for members of the LGBTQ community to feel anxiety and concern.
What is monkeypox?
Monkeypox is an illness caused by infection with the monkeypox virus—a type of virus that belongs to the same family of viruses that causes smallpox. There are two types of strains, or variants, of the monkeypox virus: West African and Congo Basin. The West African strain is responsible for the current outbreak in the US and Europe.
Where did monkeypox come from?
Monkeypox is not a new virus. First discovered in 1958 in monkeys, it was not until 1970 that a human case of monkeypox was identified. This first case was found in the Democratic Republic of Congo, and up until recently, most cases occurred in Africa. How- ever, there was a relatively small outbreak of 47 cases that occurred in the US in 2003, the first instance of monkeypox found outside of Africa. These cases were all due to contact with infected pet prairie dogs that were carrying the virus.
While the natural reservoir of monkeypox is unknown, it has been detected in many animals, including rodents and monkeys.
How is monkeypox transmitted?
Generally, it takes anywhere from 5 to 21 days to go from infection with the virus to a manifestation of symptoms. Past outbreaks could be attributed to animal-to-human contact characterized by bites, scratches, or simply touching an infected animal.
Transmission in this current outbreak is attributed primarily to prolonged skin-to-skin contact with a symptomatic person. According to the Centers for Disease Control, monkeypox can spread through direct contact with a monkeypox rash, scab, or body fluids from a person with monkeypox. Transmission also occurs by touching objects, fabrics (clothing, bedding, or towels) and surfaces that have been used by someone with monkeypox, or contact with respiratory secretions.
Monkeypox can also be spread by sharing fabrics and objects during sex that were used by a person with monkeypox and have not been disinfected. This includes bedding, towels, fetish gear, and sex toys.
What are the symptoms of monkeypox?
People who contract monkeypox usually first develop a flu-like illness characterized by fever, chills, headache, and myalgia (muscle aches). Swollen lymph nodes (lymphadenopathy) is also commonly seen with monkeypox, and this swelling distinguishes it from other viral illnesses such as smallpox.
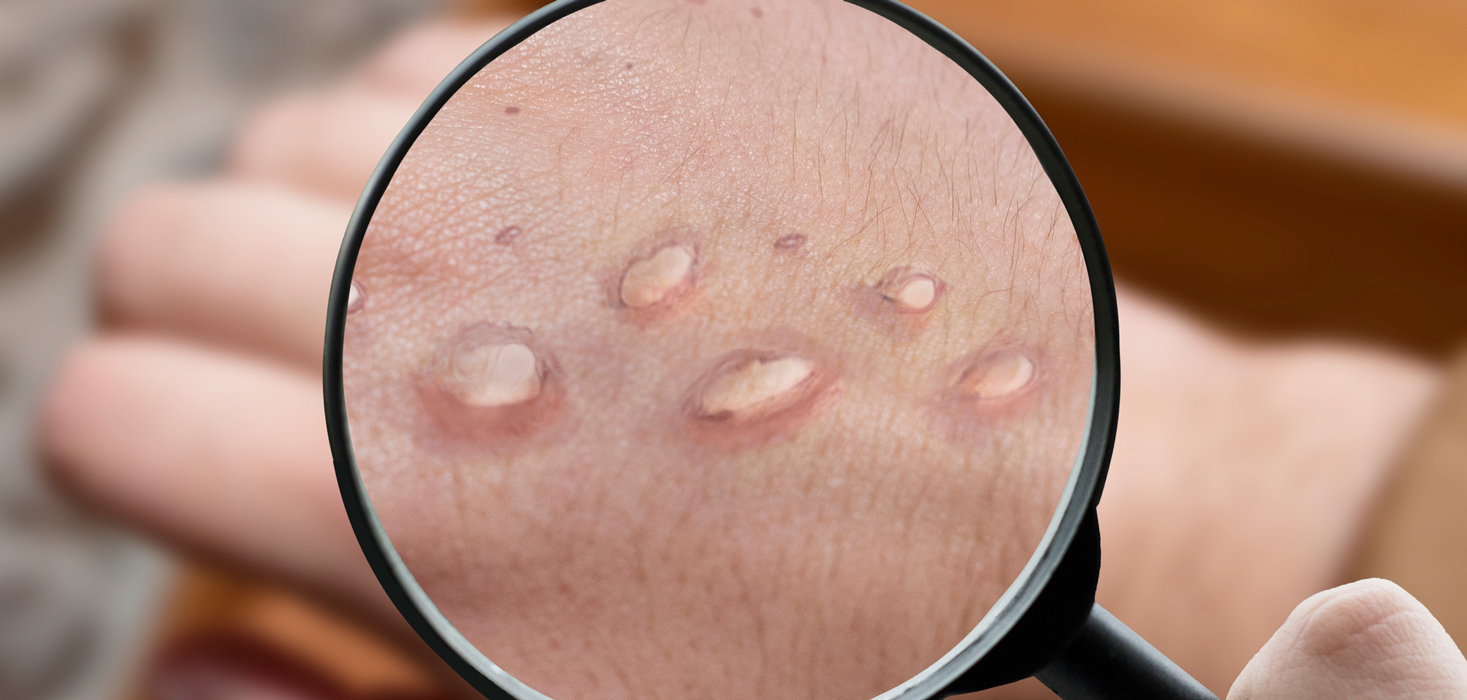
A rash typically develops within three days of the first symptoms. The rash starts off as flat or mildly raised bumps that go on to become vesicles (blisters) filled with liquid. The lesions then crust over and the scabs fall off.
It is important to note that a person with a rash or blisters is contagious until the rash has fully healed, which can take anywhere from two to four weeks. Transmission of monkeypox is possible from the time symptoms start until the scabs have fallen off and the rash is fully healed.
So monkeypox is not an STI?
Whether or not monkeypox is a sexually transmitted infection (STI) has been a confusing part of the conversation. It is important to note that monkeypox is not currently classified as an STI. This means that while it can be contracted during sexual contact of any kind, monkeypox is not thought to be spread specifically by or through semen, vaginal fluids, urine, or feces. When a disease is proven to spread through those specific body fluids, it is classified as an STI.
Researchers from the World Health Organization have found monkeypox present in body fluids such as semen. However, the current understanding remains that transmission is driven primarily by skin-to-skin and skin-to-mouth contact. This could mean that even though monkeypox can be detected in semen, there is not enough of the virus to cause another person to develop illness from it.
How can I avoid catching monkeypox?
The good news is that you may already be practicing some elements of prevention. With COVID, we have all honed our practice of excellent hand hygiene through hand washing and using alcohol-based hand sanitizer. You should continue to wash your hands to reduce your risk for contracting either illness.
Although this may go without saying, you must avoid skin-to-skin contact with anyone who has a rash that looks like monkeypox. Do not touch the rash or scabs, and do not hug, kiss, cuddle, or have sex with someone who appears to have these symptoms. Avoid sharing eating utensils or cups, and do not touch the bedding, towels, or clothes of a person with these symptoms.
Stay informed by reading public health information from reputable sources such as the CDC and our local health departments. Be aware of the prevalence of monkeypox in places you are traveling to. These resources can help you to ascertain your level of risk, guide decision-making, and keep you and your loved ones safe.
What vaccines and treatments are currently available?
Vaccines are available to prevent and treat monkeypox infection. JYNNEOS, which is the same vaccine developed to protect against smallpox, is administered as a series of two injections, with the second dose being given four weeks after the first dose.
Due to a limited local supply, the Houston Health Department currently gives priority (as of the time of this writing) to:
• People with confirmed high- or intermediate-risk contact with someone who has been diagnosed with monkeypox,
• People who attended an event or venue where there was a high risk of exposure to someone with confirmed monkeypox virus through skin-to-skin or sexual contact,
• Men over age 18 who have sex with men,
• People over age 18 whose sex partner is suspected of having monkeypox due to a rash or sores,
• People who are HIV positive or on HIV pre-exposure prophylaxis (PrEP), or
• People who have had a diagnosis of chlamydia, gonorrhea, or early syphilis within the previous three months.
Antiviral medications such as Tecovirimat have been studied in animals, but there is currently no efficacy data in humans. Such medications may be helpful in persons exposed to monkeypox who are at high risk for severe illness.
How can the LGBTQ community deal with the emotional fallout of monkeypox?
For some members of our community, monkeypox is a painful reminder of the earliest years of the AIDS epidemic when HIV was identified as a “gay disease” and the public health response was steeped in homophobia. For others dealing with the emotional fallout of COVID, adding another viral illness into the mix feels like a burden that is almost too much to bear. Increased anxiety about public gatherings and sexual contact is the last thing any of us needs.
It’s not an unreasonable approach to consider taking a brief hiatus from sexual activity and close contact with others for a time, to see how things develop. However, it’s important to not withdraw from all social contact indefinitely. Our ability to connect with others physically—through hugging, kissing, and sex—is (for many of us) an important part of having fun as well as developing and maintaining intimacy.
Daryl Shorter, MD, is a Diplomate of the American Board of Psychiatry and Neurology and is board certified in both general and addiction psychiatry. His clinical practice focuses on veteran care, and he lectures widely on LGBTQ mental health. Dr. Shorter can be reached at [email protected].











Comments